Your pump screams. Your tech glances at it, sighs, walks over, silences the alarm, checks the line, sees nothing wrong, and goes back to what they were doing. This happens three, five, maybe ten times a shift. After a few months, nobody rushes anymore. The alarm becomes background noise, like a car alarm in a parking lot that everyone has learned to ignore.
That learned indifference has a name. It's called alarm fatigue. In human hospitals, it's been classified as a patient safety crisis for over a decade. In veterinary medicine, we're just starting to talk about it.

This blog covers one section of our 2026 Veterinary IV Pump Survey. The full report includes data on equipment spending, staffing costs, fluid therapy trends, and business sustainability across 114 companion animal practices.
What alarm fatigue looks like in practice
We asked 114 companion animal practices how often pump alarms or errors interrupt their procedures.
Frequency | % of practices |
Multiple times daily | 11% |
Daily | 24% |
Weekly | 34% |
Monthly | 22% |
Rarely | 9% |
More than two-thirds of practices (69%) experience pump alarms at least weekly. Over a third (35%) deal with them daily or more.
One practice owner in Portland described it this way - her oldest pump beeps with occlusion alarms constantly, even when the line is fine. Staff have gotten so used to it that new hires think the team is ignoring equipment emergencies. They're not. The pump is just unreliable.
A practice in San Jose measured the time cost. 15 to 20 minutes per shift, per tech, just silencing alarms and resetting pumps. With four techs, that's over an hour of lost productivity every day.
Human medicine already treats this as a crisis
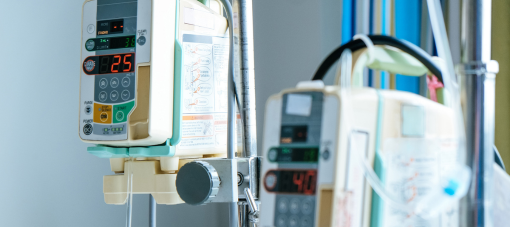
Image courtesy of Envato
The Joint Commission issued a Sentinel Event Alert on alarm fatigue in 2013, after their database recorded 98 alarm-related events in three and a half years. Eighty resulted in patient death.
Studies have found that 85% to 99% of alarm signals in hospital settings don't require any clinical intervention. One children's hospital reported 5,300 alarms in a single day, 95% of them false. The ECRI Institute has ranked alarm hazards in the top two of their annual Top 10 Health Technology Hazards list every year since they started publishing it.
Too many false alarms train clinicians to stop responding urgently. Then a real alarm goes off and the response is delayed or absent. Veterinary medicine doesn't have a Joint Commission equivalent tracking these events, but the same psychology applies and in many cases, the same pumps are being used.
The alarms that matter get buried under the ones that don't
Air-in-line alarms are the worst offender for false positives. A survey respondent in Denver described it as the most common nuisance alarm in his practice, triggering when there's no visible air in the line. Oversensitive sensors pick up micro-bubbles that pose zero clinical risk and treat them with the same urgency as a genuine air embolism threat.
Downstream occlusion alarms are a close second. A real occlusion means fluid isn't reaching the patient. But on older pumps with degraded pressure sensors, this alarm also fires when a patient shifts position or someone bumps the line.
Flow rate errors are the alarm you never want to miss. If the pump's calibration has drifted, it may be delivering fluid at a rate that doesn't match what's programmed. But if that alarm is buried under ten false occlusion alarms that shift, nobody's treating it with the urgency it deserves.
Even low-risk alarms like infusion complete and low battery add to the total count. A pump that beeps for a completed infusion, beeps for a battery, and beeps for three false occlusions in the same hour has trained your tech to stop caring about what it has to say.
This is a staff problem as much as a patient safety problem

Image courtesy of Envato
Our survey found that 76% of practices spend two or more hours per week troubleshooting equipment, and 38% spend more than five hours. At $25/hour, five hours a week of alarm-related troubleshooting costs roughly $6,500 a year. That's more than enough to buy a refurbished pump or five (depending on your model).
Beyond the dollars, constant false alarms interrupt clinical focus, erode trust in equipment, and add to the sensory load in an already demanding environment. It's the kind of thing that doesn't show up in exit interviews but absolutely contributes to the feeling that the job is relentless.
The training problem compounds this. Alarm recognition was the second-biggest training challenge for new staff in our survey (22%). One multi-location practice owner in Chicago put it well - “the hardest part isn't teaching new staff which alarms are real. It's teaching them the difference between a real problem and a temperamental pump without making them cavalier about all alarms.” When 49% of practices have all clinical staff operating pumps, not just experienced techs, that judgment call has to be made by the newest hire on the team.
What actually reduces false alarms
False alarms come from specific, fixable equipment issues.
Sensors that have drifted out of calibration (most common)
Worn mechanical components that throw off internal readings
Pumps that haven't been recalibrated to manufacturer specs in years (just like #1).
Our survey found that most practices run pumps from multiple brands acquired over time, each with different alarm logic and maintenance needs. When some are maintained and others aren't, the alarm behavior across the fleet becomes unpredictable.
The practice in San Francisco that reported "rarely" experiencing pump alarms attributed it directly to investing in refurbished units two years ago and keeping them on a maintenance schedule.
How AIV Vet addresses this
Every refurbished pump that leaves our facility in Harmans, Maryland goes through a 27-point inspection that specifically includes sensor testing, alarm calibration, worn component replacement, and full functionality verification against manufacturer specifications. When a pump passes our process, its alarms fire when they should and stay quiet when they should.
Our repair service addresses alarm-related issues directly. If your pump is giving false occlusion alarms or the air-in-line sensor has become oversensitive, that's a specific, fixable problem. Typical turnaround is 7 to 10 business days with a 6-month warranty.
For practices that want to reduce alarm sources altogether, the VetroCRI syringe pump was designed with a simpler architecture. Fewer sensors, fewer alarm types, fewer opportunities for nuisance alarms.
The goal isn't to eliminate alarms. The goal is to make every alarm mean something.
About this data
This data comes from the 2026 AIV-Vet Veterinary IV Pump Survey (114 companion animal practices across the U.S.). Human hospital alarm fatigue data is from The Joint Commission Sentinel Event Alert Issue 50 (2013) and Nyarko & Giuliano, AACN Advanced Critical Care (2025). ECRI Institute alarm hazard rankings are from their Top 10 Health Technology Hazards annual reports (2011-present).
AIV Vet has been in the veterinary equipment business for almost 2 decades. If your pumps are crying wolf and you want to fix the problem instead of living with it, we should talk.